
Formally defined, meaningful use is a term used in healthcare to outline the minimum requirements for using electronic health information and electronic health records (EHRs).
In other words, EHR meaningful use means taking steps to boost patient care with an EHR by improving the communications between patient and provider, provider and insurance, and provider to provider. Watch the video or read the transcript below to find out what meaningful use is and why you should make sure you’re compliant.
The General Intent of EHR Meaningful Use
The overall goal of meaningful use is to promote the adoption and use of EHRs. In turn, it helps to increase collaboration between clinical and public healthcare, improve patient-centric preventative care, and support the continuing development of standardized data exchanges.
Background on Meaningful Use
In 2009, the Health Information Technology for Economic and Clinical Health Act (HITECH) introduced programs designed to encourage EHR adoption. It phased in the meaningful use of EHR systems in 3 stages.
Among the other benefits of using electronic health records, one of the main methods used for encouraging adoption was a reimbursement program spanning from 2011–2015, where during that time if you were able to demonstrate meaningful use you were offered financial incentives.
Reimbursements in the Past, Financial Penalties Today
 At the start, reimbursements were given for showing meaningful use with an EHR. Now, since 2015, if you don’t show proof of meaningful use, then you’re subject to penalties for the next year on Medicare reimbursements.
At the start, reimbursements were given for showing meaningful use with an EHR. Now, since 2015, if you don’t show proof of meaningful use, then you’re subject to penalties for the next year on Medicare reimbursements.
When eligible providers don’t meet the requirements for meaningful use by 2015 they become subject to payment adjustments to their Medicare reimbursements that start at 1% per year, up to a maximum 5% annual adjustment.
Implementing EHR Meaningful Use In 3 Separate Stages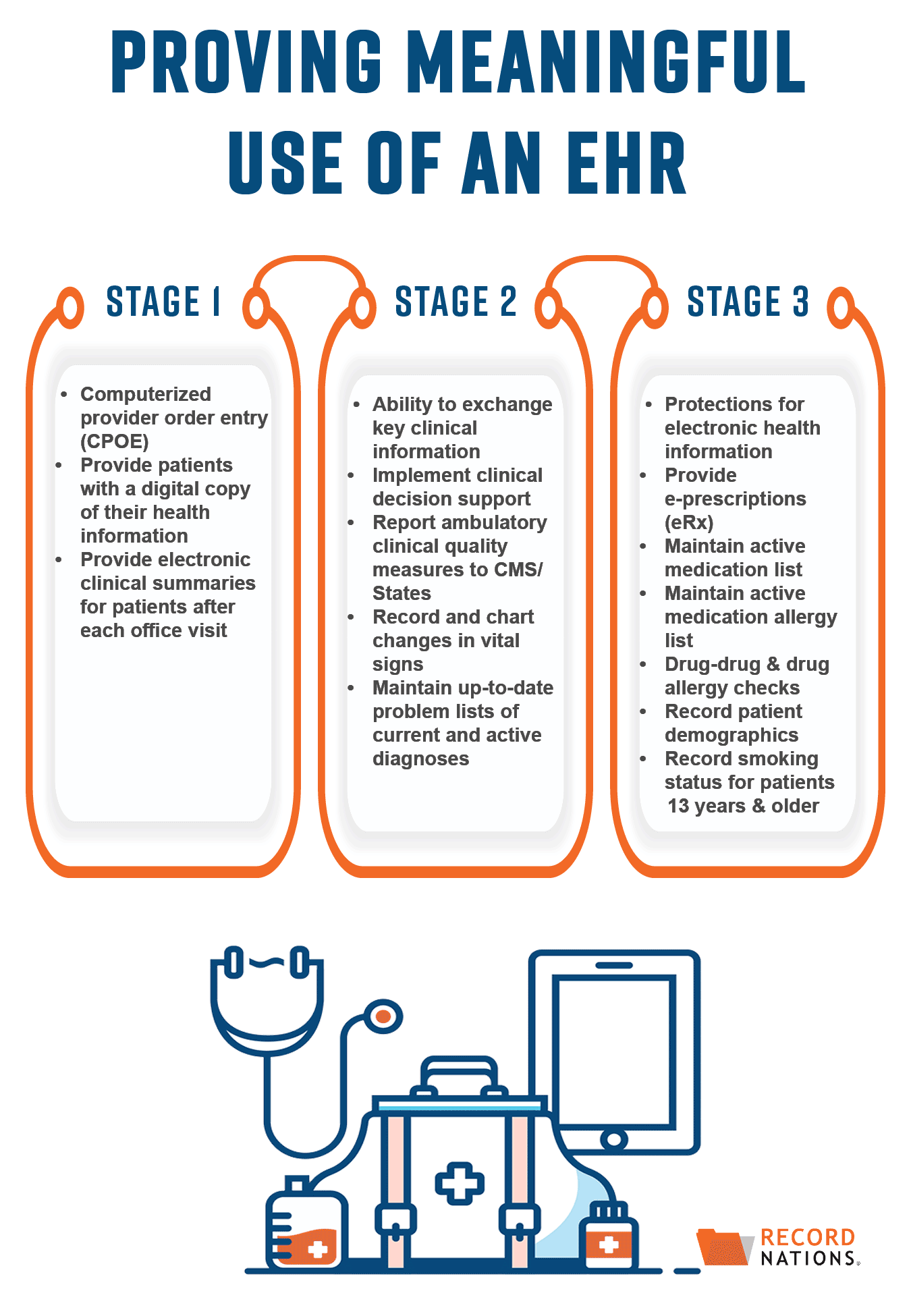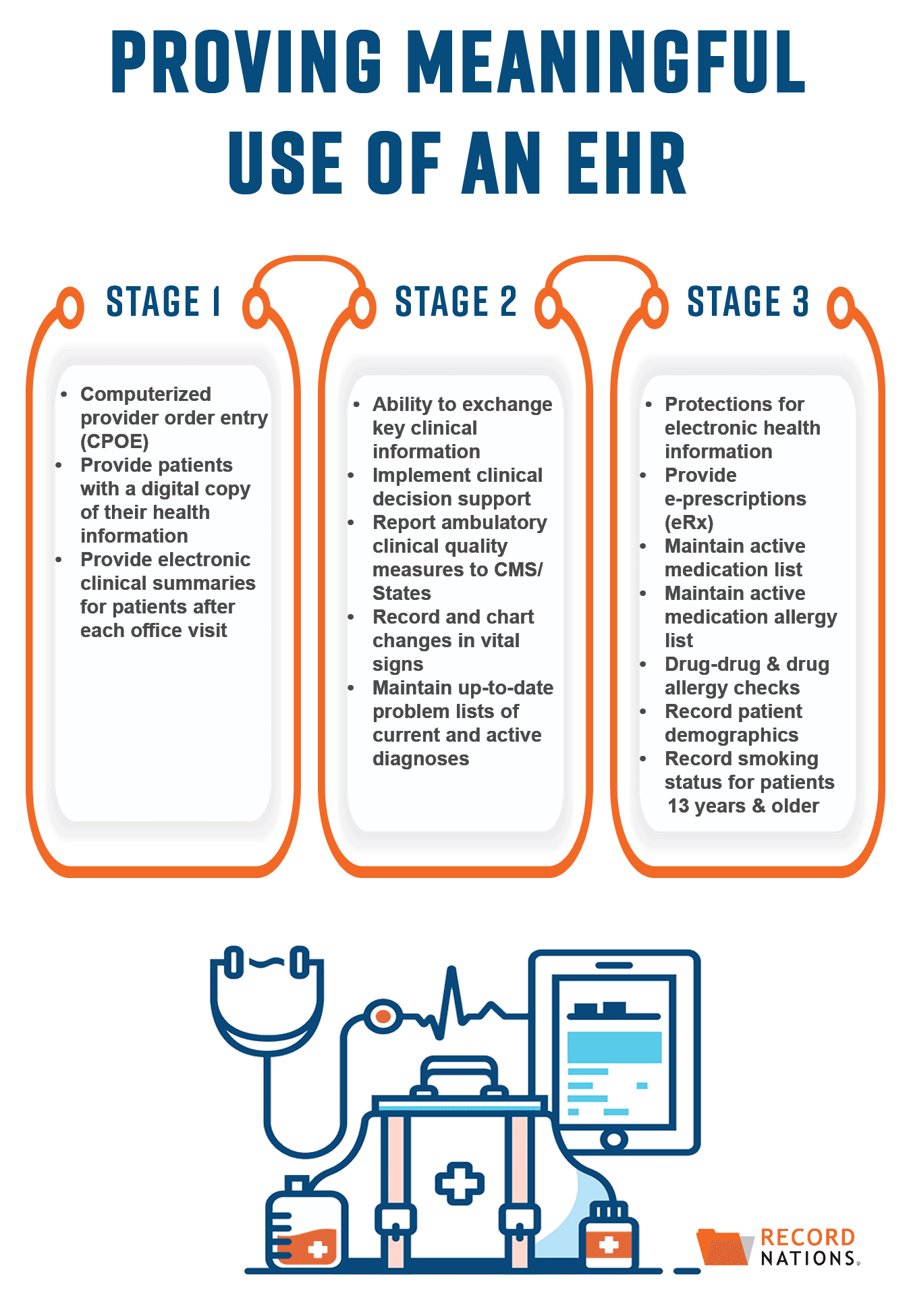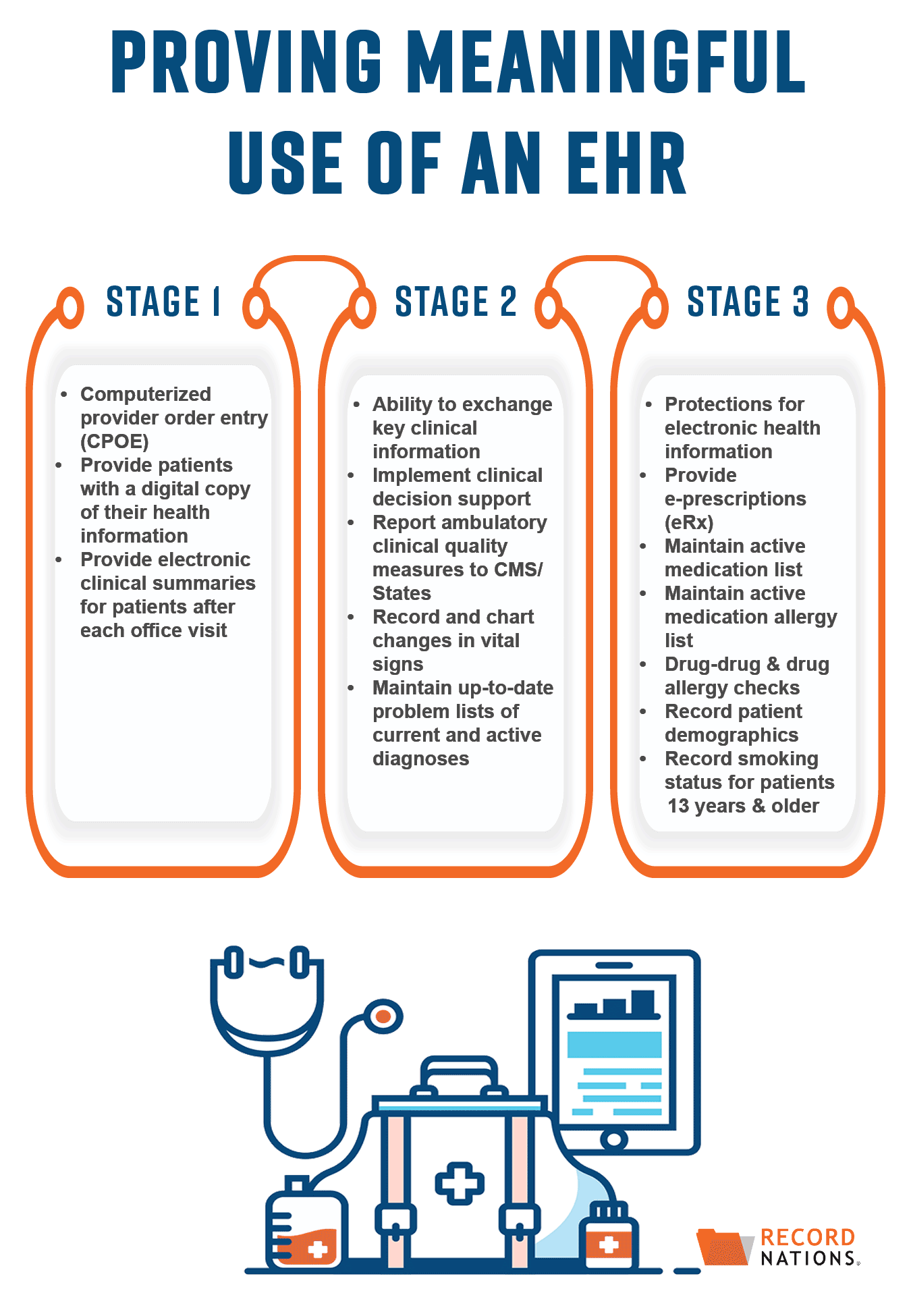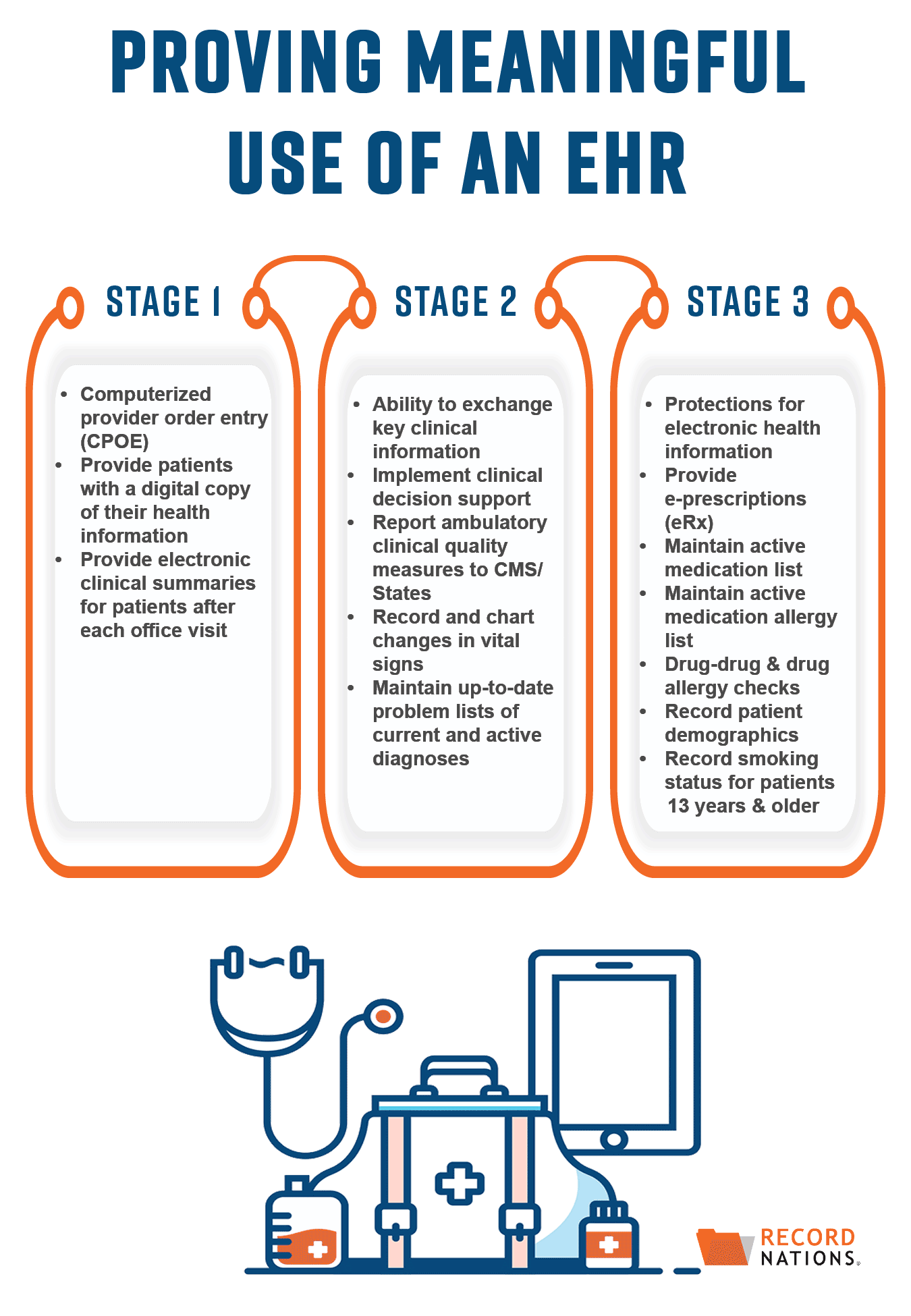
To make adopting EHRs a smoother process, the meaningful use implementation process is broken down into 3 stages:
Stage 1: Adopting Certified EHR Technologies
The main focus of Stage 1 is the promotion and implementation of certified EHR technologies. Requirements for Stage 1 are fairly straightforward—clinical data needs to be electronically captured and patients need to have the ability to access a digital copy of their health records.
Stage 2: Expanding EHR Systems to Improve Care Coordination
Stage 2 builds on the initial adoption of EHRs, this time emphasizing their meaningful use. Focusing primarily on internal needs, during Stage 2 the requirements for meaningful use expand to include the ability to exchange patient information and, as a result, improve care coordination.
Stage 3: Using More Advanced Technologies to Improve Health Outcomes
Lastly, Stage 3 finishes implementing meaningful use by taking more specific steps to improve patient health outcomes. With a larger system now in place, during Stage 3 requirements for meaningful use will include more advanced technologies like EHR system securities, e-prescriptions, and patient portals.
Final Requirements for Proving EHR Meaningful Use
There are 15 final requirements you need to meet to prove meaningful use of your EHRs. Listed based on the stage they should be implemented, these requirements include:
| STAGE 1 | STAGE 2 | STAGE 3 |
|---|---|---|
|
|
|
Improve Patient Care and Keep in Compliance Today!
Record Nations has helped healthcare providers including Children’s Medical Center and Kaiser Permanente to find EHR systems to meet their needs and CMS standards. Join them and many others by filling out our form or giving us a call at (866) 385-3706 for a free no-obligation quote from providers near you.












